What Is the Vagus Nerve and Why Does It Matter?
This post contains affiliate links. If you buy something through one of them, we may earn a small commission — at no extra cost to you. We only recommend things we'd genuinely stand behind.
The nerve you’ve never heard of is running most of the show.

You’ve probably been hearing about the vagus nerve a lot lately. Cold plunges, humming exercises, breathwork apps, half of them claim to be “stimulating your vagus nerve.” At some point it starts to sound like wellness jargon, another thing to optimize.
But the vagus nerve is worth actually understanding, because it explains a lot. Why stress hangs around long after the stressful thing is over. Why some people snap back from hard moments and others stay in it for days. Why connection can feel nourishing one day and completely draining the next.
A quick anatomy note
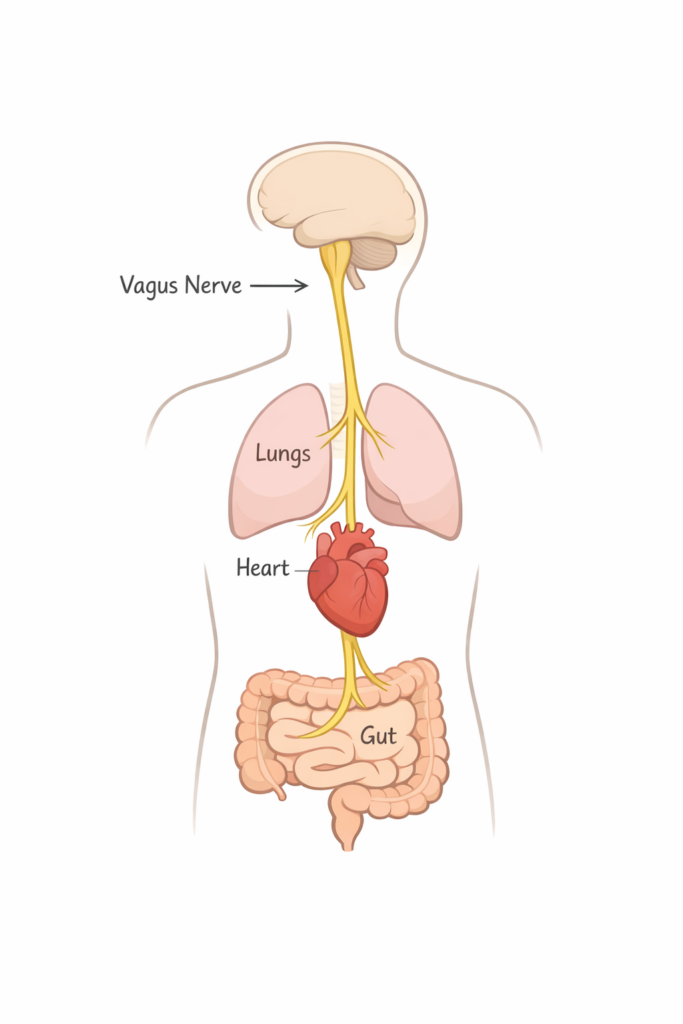
The vagus nerve is the longest of the cranial nerves. It starts at the base of your brainstem and travels down through your neck, chest, and abdomen, passing your heart, your lungs, your stomach, your gut. Vagus is Latin for “wandering,” which is accurate.
It’s the main nerve of the parasympathetic nervous system, the side of your autonomic system responsible for rest, digestion, and recovery. When people talk about “rest and digest” versus “fight or flight,” the vagus nerve is doing most of the work on the rest-and-digest side.
What surprises most people is the direction the information flows. About 80% of the vagus nerve’s fibers are sensory, sending signals upward, from your body to your brain rather than the other way around. Your gut and your heart are constantly reporting to your brain about the state of things. Your body is always talking; your brain is largely just listening and responding.
Vagal tone: what it is and why it matters
When researchers talk about vagal tone, they mean how well your vagus nerve is functioning, essentially how responsive it is. High vagal tone means your nervous system is flexible. You get activated by something stressful and you come back down. You can be in conflict and still stay present enough to work through it. Your digestion is generally fine. You recover.
Low vagal tone looks like the opposite. You get activated and stay there. Stress accumulates rather than discharging. Your gut is a mess. You feel wired and exhausted at the same time, or you swing between that and feeling emotionally numb. Social situations leave you more depleted than replenished.
Low vagal tone usually isn’t a character flaw or a lack of effort. It tends to be the result of chronic stress, early adverse experiences, or a nervous system that spent a long time in survival mode and adapted accordingly.
The social side of it
This is the part that tends to reframe things for people.
In the 1990s, neuroscientist Stephen Porges developed Polyvagal Theory, which identified a specific branch of the vagus nerve, the ventral vagal complex, that is wired for social engagement. It regulates the muscles of your face and voice, your middle ear (tuned to pick up human speech frequencies), and your capacity to read whether another person is safe.
When this system is active, you can make eye contact without it feeling like a threat. You can have a tense conversation with your partner and stay regulated enough to actually hear them. You can be in a room full of people and feel okay.
When it’s not, when you’re overwhelmed, depleted, or your system has learned that closeness means danger, the social world starts to feel exhausting or hostile in ways that are hard to explain. You know rationally that your partner isn’t attacking you. Your body doesn’t really care what you know rationally.
This is why vagus nerve health matters beyond physical wellness. It’s the physiology underneath how we relate to people.
Signs your vagal tone might be low
There’s no blood test for this, but some things worth paying attention to:
- Anxiety that feels like a background hum rather than a response to anything specific
- Staying activated after stressful events, an argument at 9am that’s still sitting in your body at 9pm
- Chronic digestive issues (the gut-brain connection runs directly through the vagus nerve)
- Emotional numbness, or difficulty accessing feelings
- Feeling socially drained in situations that shouldn’t be that draining
- Trouble hearing speech clearly in noisy environments, which is actually a vagal symptom since the middle ear muscles are vagally innervated
- Slow heart rate recovery after exercise
- A general difficulty feeling at ease, even when things are fine
None of these on their own means anything definitive. But a cluster of them, showing up persistently, is worth taking seriously.

What actually helps
Vagal tone isn’t fixed. There’s decent research showing it responds to fairly ordinary practices, most of which don’t require anything expensive.
Lengthening the exhale. Your heart rate rises slightly on the inhale and drops on the exhale, a phenomenon called respiratory sinus arrhythmia, mediated by the vagus nerve. Breathing out for longer than you breathe in (try a 4-count inhale, 6-8 count exhale) directly engages the vagal brake. Five minutes is enough to notice a difference.
Cold water on the face. Splashing cold water on your face, or briefly submerging it, triggers the diving reflex, a hard-wired vagal response that slows the heart quickly. It’s uncomfortable. It works.
Humming or gargling. The vagus nerve runs through the muscles of your throat and larynx, and vibrating those muscles activates vagal pathways. This is part of why singing in a group feels the way it does, not just emotionally but physiologically.
Being around regulated people. The ventral vagal system evolved for social co-regulation, not solo survival. Being in close contact with someone who is calm and attuned is one of the fastest ways to shift your nervous system state. It’s part of why good therapy works, and why the quality of your close relationships has such a measurable effect on health outcomes.
Vagal stimulation devices. For people who find breath-based practices hard to access, especially those with significant trauma or anxiety, devices like Sensate offer a more passive route in. It uses infrasonic resonance applied to the chest to stimulate the vagus nerve, and there’s research supporting its effectiveness for stress reduction. It’s become fairly popular among somatic therapists.

If you want to go deeper on the science, Deb Dana’s Anchored is the most readable translation of Porges’s work for a non-academic audience.
Why this is worth understanding
The nervous system doesn’t operate on logic. It operates on patterns and signals and a very old set of threat-detection systems that predate language entirely. Understanding that doesn’t make the symptoms disappear, but it does change how you relate to them. Less “what’s wrong with me,” more “what did my nervous system learn, and what might it be able to learn instead.”
The vagus nerve sits at the center of that question. It’s not magic, and working with it isn’t a quick fix. But it is a real physiological lever, and for a lot of people, understanding it is the first thing that’s made their inner experience make any kind of sense.
Read next
- Polyvagal Theory Explained: What It Means for Your Relationships
- Signs Your Nervous System Is Dysregulated
- How to Stimulate Your Vagus Nerve at Home: 12 Science-Backed Ways
SomaticGround.com explores the science of the nervous system and its connection to relationships, healing, and the embodied life. All content is for educational purposes and is not a substitute for professional medical or psychological care.